CBT for insomnia – How does it work?

What is CBT for Insomnia (CBT-I)? If you’re asking yourself that question, you’ve come to the right place! CBT for Insomnia or Cognitive Behavioral Therapy for insomnia is a branch of Cognitive Behavioral Therapy, a therapy developed in the 1960s to treat depression. Today, CBT is used as an effective way to treat a variety of disorders (anxiety, depression, eating disorders, addiction) including insomnia with CBT-I.
Sometimes referred to as CBT for sleep, CBT for insomnia is rooted in the present day and goal-orientated. CBT for insomnia focuses on finding practical solutions and coping skills. All this starts by addressing the cycles of thoughts, feelings, and behaviors found at the heart of the problem. Once these cycles have been identified, you will be able to break them with dedicated exercises.
CBT for Insomnia
CBT for insomnia uses the same principles to treat insomnia– that is a difficulty falling asleep and/or staying asleep. A standard CBT for insomnia lasts 6-8 weeks and its main goal is to break the vicious insomnia cycle. By addressing the thoughts and behaviors linked to bad sleep, it helps you restructure your sleep and put in place new habits for lasting better sleep. But that may still seem a little theoretical. Let’s take a look at how it works in practice:
Cognitive Behavioral Therapy for Insomnia can be broken down into 4 main blocks:
What is CBT for insomnia? 1. Stimulus Control
Trouble falling asleep and waking up during the night mean that the ratio of time spent in bed awake/ asleep is off-kilter. Little by little, a mental association between the bed, or bedroom and being awake is formed.
Eventually, a vicious insomnia cycle is established. The more time spent awake in bed, the more stressful it becomes. And the more stressed someone becomes, the more difficult it is to sleep.
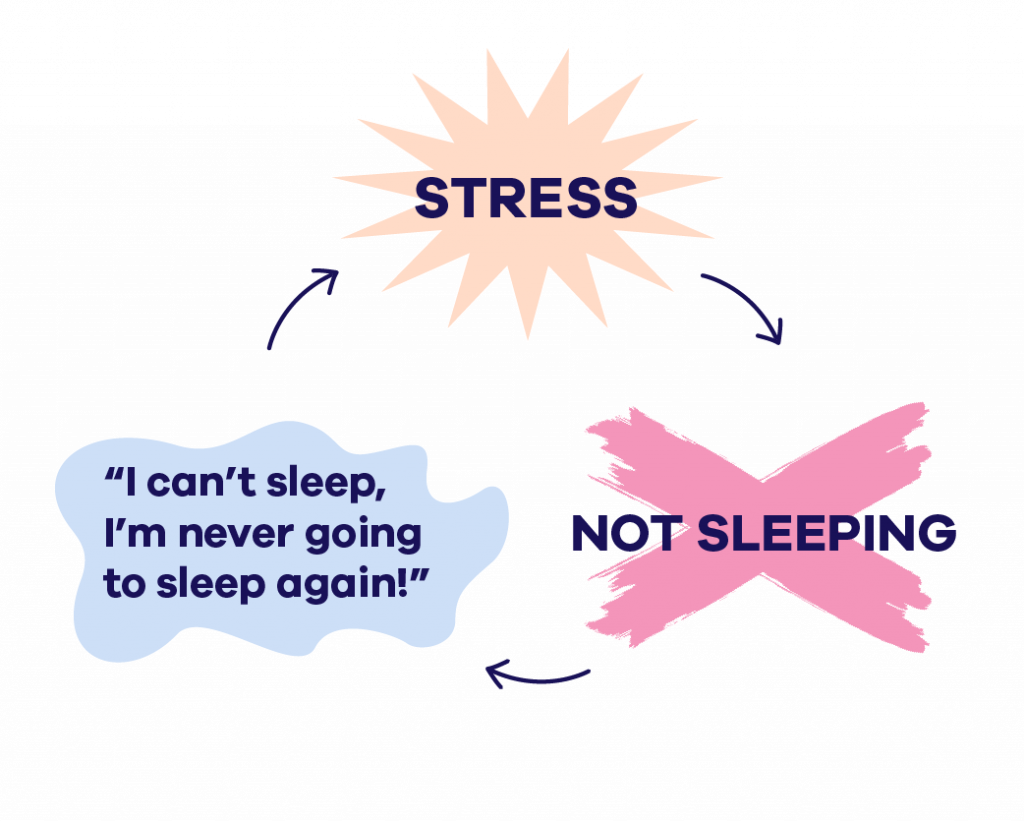
The part of CBT-I known as “Stimulus Control” aims to break these negative bed-awake associations, and put in place positive bed-sleep thinking. This is done in a very practical way, through a set of rules:
- No activity in bed except sleep
- Go to bed only when tired
- No naps during the day
- If it takes more than 20 minutes to fall asleep or fall back asleep once you wake up during the night, get out of bed and only return once sleepy.
What is CBT for insomnia? 2. Sleep Consolidation
Now we come one of the most important blocks of CBT for Insomnia: Sleep consolidation, which may sound counterintuitive, but is proven effective against chronic insomnia. As we mentioned above, for insomniacs, the ratio of time spent in bed awake/ asleep is off-balance. The aim here is set that right by maximizing sleep pressure- put simply how sleepy you feel- by pushing back bedtime. Once you’re in bed you should be so sleepy and fall asleep more easily and more likely to sleep in one long, consolidated stretch.
So how does it work?
Let’s say that you go to bed every night at 11pm and wake up every morning at 7am, but you don’t actually fall asleep until 1 am. When you do fall asleep, your sleep is fragmented. Your average night would look a little like this:
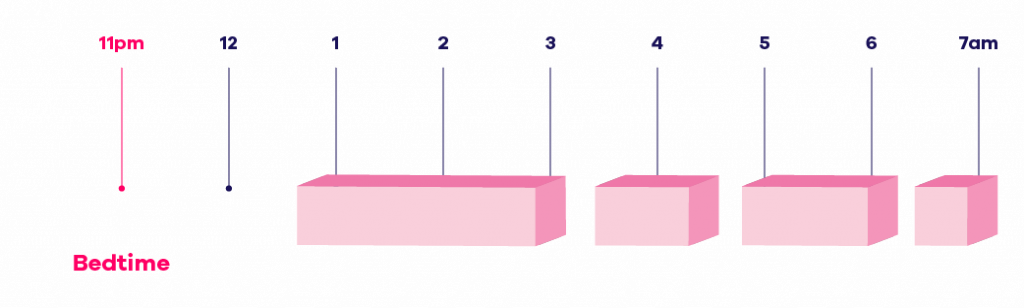
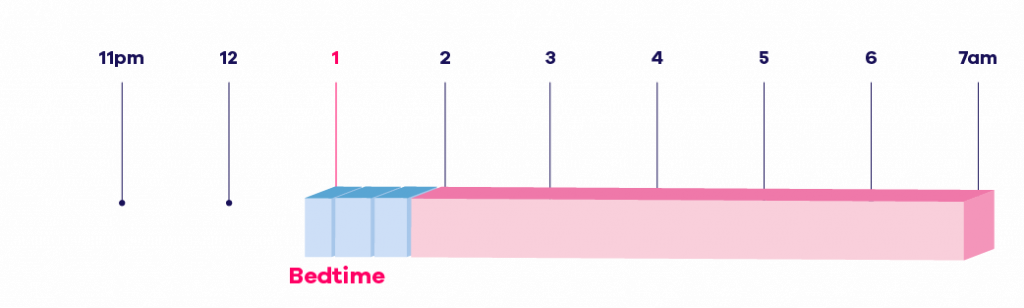
The first step of sleep consolidation is to work out your total sleep time, taking out the times you woke up and the time you took to fall asleep. In this example, your total sleep time is 5 hours. These 5 hours are then taken away from your wake-up time (here 7am) making your initial bedtime 2 am:
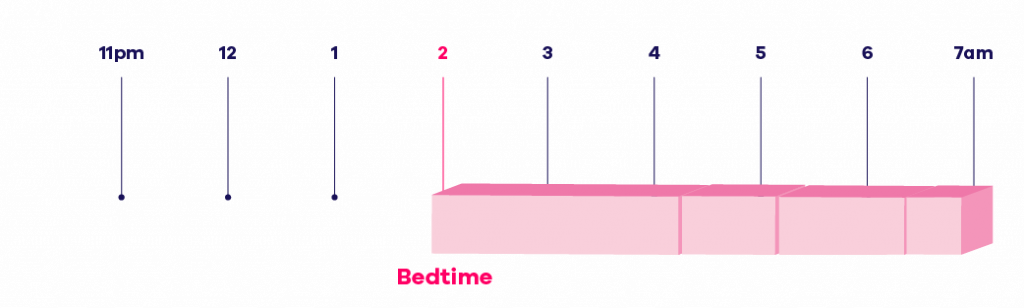
Little by little, your sleep should become consolidated into one uninterrupted block. Once this has been achieved, bedtime will be brought forward in small increments, adding time onto your consolidated total sleep time:
There’s no denying that sleep consolidation is tough but CBT for insomnia has shown this method to be effective, The results are there, you’ve just got to stick with it.
What is CBT for insomnia? 3. Sleep Hygiene
Sleep hygiene concerns pre-bedtime behavior and environment. So basically, where you sleep and what you do before bed. This means avoiding over-stimulation, stimulating substances like caffeine, nicotine, and choosing relaxing, screen-free activities like reading a book, meditating. These small changes may seem like basic common sense, but go a long way in building a lasting, healthier sleep routine.
What is CBT for insomnia? 4. Cognitive Therapy
One of the biggest barriers for insomnia sufferers is sleep-related anxiety. As we mentioned above, sleep is so problematic that even the idea of bed becomes stressful which in turn makes it harder to sleep.
The role of cognitive therapy for insomnia here is to unmask the sleep bogeyman, by learning about your sleep. Also, rationalizing sleep-based fears and stress, by keeping a thoughts journal or filling out inventories.
So, what’s the catch?
Traditional CBT, as great as it is, isn’t without its shortcomings. The number of practitioners is limited, so it can be hard to get access to. Besides, if it isn’t covered by your insurer, it can be costly.
That’s perhaps why more and more people are turning to online CBT for insomnia programs. There’s no denying that this digital revolution has opened up Cognitive Behavioral Therapy for insomnia to a larger population.
Digital and traditional CBT for insomnia have one flaw in common. They both rely on a subjective view of sleep. The insomnia sufferer is asked to keep a sleep journal, noting down/ typing up their sleep time, nocturnal awakenings, how long it took to fall asleep.
Even for good sleepers, it’s near impossible to have a precise idea of these figures, and for sufferers of insomnia, this declarative necessity seems nearly counterintuitive.
As we’ve seen above, people with insomnia don’t necessarily have an objective view of their sleep, and this kind of rigorous timekeeping may add to sleep-related stress.
This article is part of our series: CBT-I: What you need to know. You’ll find a list of all the articles in the series by clicking on the link.
Up Next: CBT-I: Week by Week
Discover your sleeper profile with this sleep test
Start



